|
12/10/2023 0 Comments Pacemaker failure to capture ekg 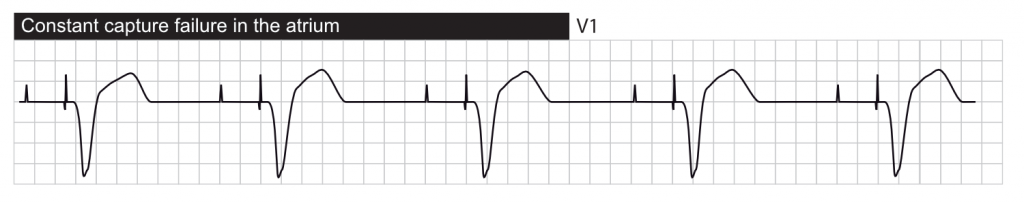
In patients presenting with symptoms suspicious for pacemaker syndrome (hypotension, shortness of breath, dizziness, most commonly in an intermittent pattern), atrioventricular activation sequence and presence of ventriculoatrial conduction should be assessed. If artifacts limit interpretation, comparing multiple simultaneous ECG leads may be helpful ( Figure 43). Underlying conduction blocks may mimic paced beats ( Figures 41-42). Atrial pacing preserves normal ventricular activation, so it may be interpreted without interference from the device. The spikes after the 3rd and 5th beats are artifacts.ĮCG analysis should always include assessment of QRS and ST-T, even in patients with paced rhythms. An underlying, slow regular atrial rhythm is seen in V2 and V5. VVI pacing without retrograde conduction. Underlying rhythm should be identified: atrial fibrillation/flutter may be difficult to recognize with asynchronous pacing, but still pose a thromboembolic risk ( Figures 39-40). If no spikes are seen, the rhythm is likely not related to pacing and patient-related issues should be suspected ( Figures 35-38). Transient changes in rhythm may elucidate the mechanism of a suspected malfunction ( Figure 34).īoth atrial and ventricular tachyarrhythmias may raise the concern of device malfunction. Device interrogation is strongly recommended (Ip, 2011). The differential is usually difficult based on surface ECG alone, unless initiation and termination can be clearly identified. Rate response function may also cause transient increase in pacing rate. 
If pacing spikes are seen during tachycardia, most common causes are atrial tachyarrhythmia tracked by the pacemaker, or true PM mediated tachycardia (caused by retrograde conduction or atrial oversensing of ventricular events, leading to endless loop tachycardia). (B) Isorhythmic dissociation between sinus rhythm and VVI pacing – close inspection of the PR intervals reveals that the atrial activity is not tracked This device is a VVI pacemaker in a patient with complete heart block. 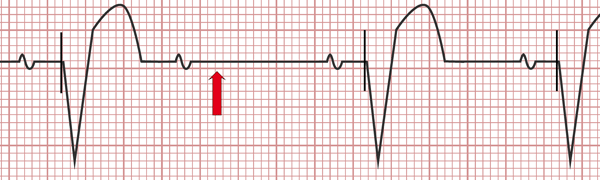
However, the ventricular rate is completely regular despite variable P-P intervals. (A) In III and aVF it may appear that the atrial activity is tracked to the ventricles. Pacing mode may be difficult to identify from surface ECG. It may change due to algorithms trying to minimize right ventricular stimulation ( Figures 30-32), rate smoothing function ( Figure 33), or arrhythmia – mainly, atrial fibrillation ( Israel, 2002). Occasionally, pacing mode may be difficult to identify based solely on the ECG ( Figure 29). Identification of the pacing site is crucial to prove appropriate device function ( Figures 25-28). Variable signal morphology may be caused by fusion beats (when the resulting signal morphology is the sum of activation from the pacemaker and spontaneous/conducted activation) or pseudofusion beats (pacing occurs when the myocardium is already refractory from spontaneous/conducted activation, Figures 22-24). „Anticipated” spikes may be missing due to very small variations in heart rate, inhibiting demand pacing ( Figure 21). Spike morphology may be affected be automatic signal gain function of the ECG system or issues with digital sampling ( Figure 20). In addition, myocardial depolarization has a vector, which may be isoelectric in certain leads, or may be delayed by intraatrial or intraventricular conduction delay, suggesting ineffective stimulation ( Figure 19). 
With ubiquity of bipolar systems, spikes may be difficult to identify ( Figure 18). P/QRS morphology, timing and response to pacing spikes should be addressed, when analyzing the ECG. Unexpected findings with normal device functionĬertain artifacts or interaction of pacemaker algorithms with underlying rhythm may lead to electrocardiographic findings, which may be difficult to distinguish from abnormal function ( Balachander, 2011). 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
